Page Under Maintenance
This page is currently under maintenance.
Please communicate at the hospital help desk for assistance.
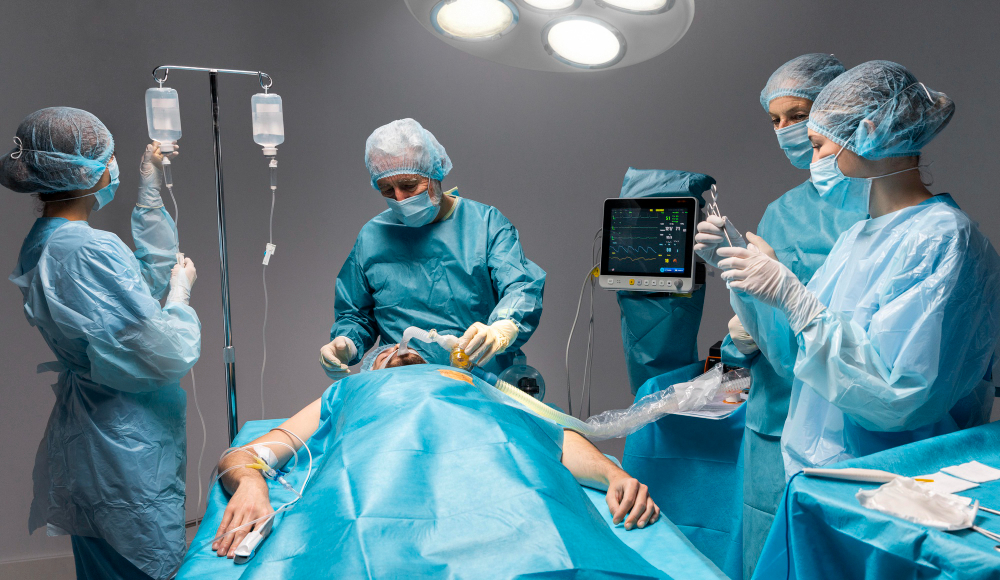
By making treatments safer, quicker, and less invasive, laparoscopy has revolutionized modern surgery. Laparoscopy, in contrast to open surgery, requires small incisions, sophisticated surgical instruments, and an internal visualization camera. Preparing for a minimally invasive operation, such as a laparoscopic cholecystectomy, is crucial to a successful outcome and a quicker recovery.
This detailed patient guide covers the advantages of laparoscopic surgery, how to prepare for the procedure, what to expect on the day of surgery, and the potential long-term side effects. It also teaches you how to select a laparoscopic surgeon for a safe and efficient surgical procedure.
During laparoscopic surgery, tiny incisions are made to insert a laparoscope, a narrow tube with a high-definition camera, into the belly. Using specialized tools, the surgeon may execute the procedure with extraordinary precision thanks to this camera's real-time video transmission to a monitor.
Because minimally invasive procedures result in less pain, less scars, and quicker recovery times than open surgery, patients prefer them. Smaller incisions result in less tissue damage, which shortens hospital stays, lowers blood loss, and lowers the chance of infection. In the end, patients can resume their regular activities faster, which lessens the disruption to their life during the surgical procedure.
Minimally invasive procedures lessen the overall financial, psychological, and physical costs of surgery for the majority of patients. Hospital stays are reduced, recovery times are much shorter, and the likelihood of complications is generally lower. Laparoscopy has emerged as the gold standard for treatments such as appendectomy, gallbladder removal, hernia repair, and gynecological surgeries.
There are advantages of laparoscopic surgery that go beyond aesthetics. The method and technologies employed greatly enhance results and patient comfort in general.
Minimally invasive surgery, adherence to pre- and post-discharge plans, and improved recovery after surgery (ERAS) procedures can all lead to quicker healing and shorter hospital stays. Using smaller incisions to lower the risk of trauma and infection, early mobilization, efficient pain treatment, keeping a normal body temperature, and adhering to explicit post-discharge instructions for wound care, diet, and activity are all important tactics.
Tissue injury is low when small incisions are made rather than massive wounds. Instead of weeks, patients typically recover in a matter of days. This results in lower hospital costs and a quicker return to normal activities.
Use silicone sheets or petroleum jelly to keep the incision moist and shield it from the sun to minimize pain and scarring. After the scar has healed, you can control its appearance and discomfort by using silicone gels or sheets, massage, and sun protection. See a physician about prescription creams, injections, or procedures like dermabrasion if you have severe scarring or ongoing pain.
Because there is less internal trauma following laparoscopic surgery, there is less pain afterward. Over time, the tiny scars, which are frequently smaller than one centimeter, become hardly noticeable. Soon after surgery, patients feel more comfortable going back to their regular lives.
Maintain proper hygiene, such as frequent hand washing and safe food handling, to reduce the risk of infection and consequences. Keep your immunizations current and stay away from sick people. These actions can stop the spread of infectious diseases and are essential for one's own health.
Germs have a lesser point of entrance when incisions are smaller. This significantly lowers the danger of hernias, wound infections, and other issues that are frequently connected to open surgery.
Technological developments like robotics and artificial intelligence (AI), which provide surgeons more dexterity, improved visualization, and tremor filtration, improve surgical precision and result in better outcomes.
Surgeons can operate with unparalleled accuracy thanks to the laparoscope's high-definition imaging and magnification. This increases organ preservation, lessens bleeding during surgery, and improves long-term results.
Laparoscopy preparation is just as crucial as the actual procedure. It guarantees that the demands of the operation are met by your body, mind, and way of life.
A pre-surgery medical examination is a check-up conducted prior to a procedure to determine whether a patient is healthy enough for surgery and to detect any potential dangers.
Your surgeon might prescribe tests like:
Special preoperative evaluations may be necessary for patients with diabetes, hypertension, or respiratory disorders.
Maintain a current list of all the substances you take, carefully read label directions, and always consult a healthcare provider before taking anything new in order to adhere to prescription and supplement standards.
Your surgeon could request that you discontinue or modify certain drugs, like:
Everything you take, even over-the-counter medications, should always be disclosed.
The morning before surgery, solid food is typically prohibited. Clear liquids, such as water or clear broth, may be consumed up to two hours before to the treatment. What should you avoid eating three days prior to surgery? To lessen bloating and improve digestion, stay away from heavy, fatty foods, alcohol, spicy foods, and processed snacks.
You might have to do the following:
This lessens the chance of anesthesia and keeps nausea at bay while recuperating.
Mentality, lifestyle, and quick coping strategies are all part of psychological preparation for lowering anxiety. Important tactics include thinking positively, controlling stress with relaxation methods like deep breathing and mindfulness, and using knowledge and imagery to get ready for particular occasions.
Before surgery, a lot of individuals experience anxiety. Fear can be lessened by being honest with your surgeon about the operation, risks, and results. Deep breathing, meditation, or guided relaxation can help certain patients.
You can feel more prepared and less anxious if you know what to expect on the day of the procedure.
A critical, multi-phase procedure intended to guarantee patient safety and maximize health outcomes prior to, during, and following surgery is preoperative admission and final examinations.
Upon entrance, the group will:
The anesthesiologist will meet you and address any last questions you may have.
Surgery is a multistage medical procedure that is usually separated into three stages: preoperative, operational, and postoperative.
Following the administration of anesthesia:
This minimally intrusive method guarantees accurate and effective surgery.
The laparoscopic cholecystectomy procedure, which removes the gallbladder because of stones or infection, is one of the most popular laparoscopic surgeries.
Patients require the surgery when they encounter:
After a laparoscopic treatment, most patients resume their regular activities within 1-2 weeks, whereas recovery from gallbladder removal usually takes 4-6 weeks. Pain management, a low-fat diet, hydration, and a gradual increase in physical activity, such as walking, are all part of the first recovery. Patients should adhere to all post-operative recommendations and refrain from driving, hard lifting, and intense activities for at least a few weeks.
The majority of patients return home the same day or the following day. Within hours, regular walking is advised. At first, light meals are permitted, and then the regular diet is gradually restored. In three to seven days, many people return to work.
While laparoscopy is safe, understanding the long-term side effects of laparoscopic surgery allows you to make more informed judgments.
The liver distributes bile straight into the small intestine following gallbladder removal, which may make it more difficult to digest foods high in fat and cause symptoms including gas, bloating, and diarrhea.
Certain patients might encounter:
Usually, these become better in a matter of weeks or months.
Scar tissue adhesions are bands of scar tissue that develop between normally unconnected internal body surfaces, causing tissues and organs to adhere to one another. They frequently develop as a part of the body's healing process following surgery, trauma, or inflammation.
Adhesions may develop internally over time, albeit they are less frequent than open surgery. Although they rarely result in consequences, they should be closely watched if symptoms like sporadic stomach pain appear.
A protrusion at or close to a prior surgical incision site brought on by a weakening in the abdominal wall is known as an incisional hernia. Premature physical activity, obesity, smoking, diabetes, steroid use, pregnancy, and wound infections are risk factors.
Hernias can occasionally result from weakening at the sites of incision. This can be avoided by keeping a healthy weight and refraining from heavy lifting during the early stages of rehabilitation.
Complications including persistent infection, bile duct damage, or chronic pain are very uncommon but can happen depending on how complicated the procedure is.
Immediate monitoring, appropriate wound care, and adhering to doctor recommendations for activity and pain control are all part of post-surgery care.
Long-term success is ensured by appropriate recuperation procedures.
A combination of physical and psychological methods, such as mild exercise, heat/cold therapy, and stress-reduction strategies like meditation, are used to alleviate pain.
Mild discomfort is typical. Analgesics may be prescribed by your physician. Regular walking can ease the discomfort caused by gas.
Before returning to a regular diet following laparoscopic surgery, begin with a clear liquid diet and gradually move to soft, easily digested meals like soups, yogurt, and pureed fruits and vegetables.
To begin with:
First, stay away from spicy and oily foods.
Start with tiny, incremental efforts to resume regular tasks, like light chores and basic self-care, while taking regular breaks and paying attention to your body.
Typical patients:
Pay close attention to what your surgeon says.
Related: How Safe is Laparoscopy? Minimizing Risks in Surgery
Surgery is safer, quicker, and more comfortable using laparoscopy. You can make confident healthcare decisions if you know the advantages of laparoscopic surgery, what happens during a laparoscopic cholecystectomy procedure, and the long-term side effects of laparoscopic surgery. Patients can anticipate great results and a speedy recovery with the right planning and direction from the laparoscopic surgeon.
Depending on their health, it is safe for the majority of people, including seniors and children.
The majority of patients have a good recovery, although occasionally there may be small problems like scar tissue or alterations in the digestive system.
Examine hospital accreditation, experience, reputation, patient testimonials, and minimally invasive surgery specialization.