Our Expertise
Varicose Veins
Our physicians performed the first documented Laser treatment of Varicose Veins in the country on 6th January 2003 at Jaslok Hospital. Thousands of our patients have benefitted from non-surgical methods of treatment of Varicose veins, using various techniques such as Laser, Radiofrequency ablation and Foam Sclerotherapy, MOCA, Glue treatment and Ambulatory Phlebectomy. Patients from all over India and from over 30 countries have visited Doctor House Vein Care Centre for valuable expert opinion on Varicose veins, and treatment. We have had the privilege of treating Captains of Industry, Leading Politicians, Film and Television artists and leaders of Civil society. However, we are very strict about valuing patient confidentiality at our centre, and no patient information is shared without the express consent of our patients.
At our centre, each patient undergoes a thorough evaluation for his/her vein condition, including a detailed clinical evaluation followed by Ultrasound tests, and other examinations if required. The proposed method of treatment is individualized for each patient, as many patients will only need conservative methods of management such as medications and compression stockings. Those with advanced or painful disease are given the option of opting for advanced non-surgical therapy. Our well experienced assistant doctors and nurses (male and female) help in following up and managing our patients after treatment procedures are completed. Recently many of the Insurance Companies have approved Varicose veins treatment.
_______________________________________________________________________________________
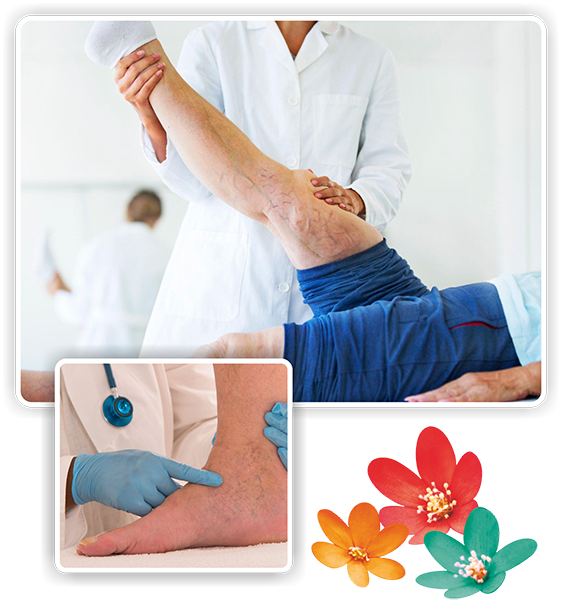
What are Varicose Veins ?
Varicose veins are enlarged, tortuous veins seen in the legs and feet. They may occur as small spider veins or may become extremely enlarged. Varicose veins progress over a period of time, later giving rise to symptoms and may be responsible for multiple complications in some patients.
_______________________________________________________________________________________
Symptoms of Venous Veins insufficiency:
- Leg pain, aching or cramping
- Burning or itching of the skin
- Leg or ankle swelling
- Heaviness of legs
- Swelling in the ankles
- Open wounds or sores
- Skin pigmentation around the ankles
- Skin discoloration or texture changes
- Venous ulcers (non-healing wounds) around the ankles
- Rupture of veins and bleeding
- Development of clot formation (thrombosis)
_______________________________________________________________________________________
Risk Factor of Venous Veins insufficiency:
- Gender
- Age
- Heredity
- Pregnancy
- Standing occupation
- Obesity
- Prior injury or surgery
- Sedentary lifestyle
_______________________________________________________________________________________
Why Do Varicose Veins Develop?
Leg veins carry blood from the legs to the heart against gravity. These veins have many one-way valves, so that the blood goes up towards the heart only, and not downwards. If these valves are damaged, on standing up or sitting, the blood in the veins will now flow down into the legs due to the effect of gravity, leading to gradual dilatation and enlargement of the veins, leading to Varicose Veins.
What Differentiates Us
Key Technologies
Methods of treatment
Routine Endovenous Treatment Procedures
There are several methods by which varicose veins can be treated. The specific procedure or combination of procedures recommended is based upon the severity of the condition. Some treatment options include the following:
- Methods of Treatment
- Laser Treatment
- Radio Frequency Ablation
- Foam Sclerotherapy
- Glue Therapy
- MOCA
- Microwave Laser
- Hi Intensity Focused Ultrasound (HIFU)
- Steam Ablation
_______________________________________________________________________________________
Laser Treatment
Endovenous laser treatment can treat larger varicose veins in the legs. A laser fibre is passed through a thin tube (catheter) into the vein. While doing this, the doctor watches the vein on a duplex ultrasound screen.
_______________________________________________________________________________________
Radio Frequency Ablation
Radiofrequency ablation (RFA) is a procedure that may reduce pain. A radio wave produces an electrical current, which heats up a small area of nerve tissue. This curbs pain signals from that specific area.
_______________________________________________________________________________________
Foam Sclerotherapy
Foam sclerotherapy is a minimally invasive technique for men and women to eliminate unsightly varicose veins and spider veins. The procedure involves injecting a foam sclerosant in a blood vessel to close it.
_______________________________________________________________________________________
Glue Therapy
Varicose vein glue is one of the most advanced permanent treatments for varicose veins. During treatment with the VenaSeal system, which is used for the gluing of veins, a disposable set is placed directly into the affected vein under sterile conditions.
_______________________________________________________________________________________
MOCA
Mechanico Chemical Ablation (MOCA),(Clarivein-USA or Flebogrif-Poland) is a newly developed, non-thermal, non-tumescent technique for the treatment of varicose veins.It is an alternative method for closing off a vein causing chronic venous reflux, restless leg syndrome, itching and pain
_______________________________________________________________________________________
Microwave Laser
Microwave Ablation (EVMWA) appears to be another extremely safe and effective technique for the treatment of varicose veins. Endovenous Microwave Varicose Veins Treatment is the latest treatment for leg varicose veins. It uses heat to permanently destroy refluxing veins. Closing these veins forces venous blood to flow the right way again.
_______________________________________________________________________________________
High Intensity Focused Ultrasound
High-Intensity Focused Ultrasound (HIFU) may prove to be the next disruptive technology in the treatment of varicose veins and venous reflux disease. It is totally non-invasive, with ultrasound energy being beamed from a transducer applied to the skin above the vein.
_______________________________________________________________________________________
Steam Ablation
Endovenous Steam Ablation (EVSA) is a new method of thermal vein ablation that works by heating the veins with steam to a maximum temperature of 120 degrees centigrade. Steam is ejected into the treated vein from two areas at the tip of the catheter
_______________________________________________________________________________________
What are DVT?
Deep Vein Thrombosis (DVT) is a serious condition that occurs when a blood clot forms in a vein located deep inside your body. A blood clot is a clump of blood that’s turned to a solid-state. In some patients, severe DVT can lead to a clot traveling into the lungs, causing Acute Pulmonary Thromboembolism, which can be fatal. In others, if the DVT persists, it may lead to chronic swelling of the legs, with ulcers and the development of varicose veins.
Deep Vein Thrombosis can develop if you have certain medical conditions that affect how your blood clots. It can also happen if you don't move for a long time, such as after surgery or an accident, or when you're confined to bed.
It is now possible to treat severe DVT by means of interventional techniques, by injecting clot-dissolving drugs such as Urokinase directly into the clot. This leads to a rapid decrease in the swelling of the legs, and also prevents pulmonary embolism. In cases where pulmonary embolism has already occurred, or likely, an IVC metal filter can be positioned to prevent further complications.
_______________________________________________________________________________________
DVT Symptoms
According to the Centers for Disease Control and Prevention (CDC) Trusted Source, symptoms of DVT only occur in about half of the people who have this condition. Common symptoms include:
- Swelling in your foot, ankle, or leg, usually on one side
- Cramping pain in your affected leg that usually begins in your calf
- Severe, unexplained pain in your foot and ankle
- An area of skin that feels warmer than the skin on the surrounding areas
- The skin over the affected area turning pale or a reddish or bluish color
_______________________________________________________________________________________
Blood clot in leg vein
A blood clot in a leg vein may cause pain, warmth, and tenderness in the affected area.
_______________________________________________________________________________________
WHAT is gangrene ?
Gangrene is defined as a localized death and decomposition of body tissue, resulting from obstructed circulation or bacterial infection. Foot gangrene, as a part of diabetes or atherosclerosis, has become a major medical problem. When gangrene sets in, an amputation needs to be performed.
An amputation, one of the oldest surgical procedures, usually refers to the surgical removal of the whole or part of a lower or upper extremity - a foot/leg or a hand/arm. Amputation, however, should be attempted only after all forms of treatment have been exhausted. The vast majority of amputations are performed due to vascular disease. Blockages in the arteries result in insufficient blood supply to the limb.
When narrowing or hardening of the arteries becomes severe, gangrene develops and amputation may be the only option Because diabetes can cause vascular blockages, about 30 - 40 percent of amputations are performed in diabetics. The estimated risk for major amputation in diabetics is 15 to 40 times higher than the general population.
In fact, amputations are an extremely feared complication of diabetes as diabetics also often lose their protective sensation and may form ulcerative complications, such as osteomyelitis - an acute or chronic inflammatory process of the bone and its structures. If Gangrene is left untreated - depending on the severity of someone's condition - infection can develop and threaten the life of the patient. If amputation is not performed, in these circumstances gangrene can be fatal.
_______________________________________________________________________________________
How Do You Prevent Gangrene From Occurring?
One of the earliest signs of decreased blood supply to the legs is pain or discomfort in the legs on walking. This pain decreases as soon as the person stops exercise. This is called intermittent claudication and is due to an imbalance between the blood supply to the legs and the demand of the muscles during exercise. As the severity of the blockages increases, the distance that the person can walk decreases. With a severe degree of narrowing of the blood vessels, the person can develop pain in the legs even during rest. If the blood vessel closes completely, and there is inadequate flow via small bypass (collateral) arteries, then the tissue of the legs will die, resulting in Gangrene.
If diagnosed in the early stages, certain medications such as Pentoxyphylline and Cilostazol are used, which help to deliver more blood supply to the tissues. In later stages, with advanced blockages, either an Interventional technique such as Balloon Angioplasty and/or Stent Placement may be used to open up the narrowed and blocked arteries, and to restore blood supply to the legs. With advances in technology and newer equipment, even advanced degrees of blockages can be opened up by these non-surgical techniques in many instances. Sometimes, when Interventional techniques are not feasible, then open Vascular Surgery may be performed using a bypass channel.
It is important to note that once gangrene has developed, then the dead tissue has to be removed surgically. In such cases, the role of Interventional techniques is to restore the blood supply as far as possible and prevent the gangrene from spreading, leading to amputation of a major part of the limb. For example, if the gangrene has already affected the Great toe of the foot, then the great toe will need to be removed surgically. However, opening up the blocked artery below the knee will help to prevent the spread of Gangrene further into the foot; if this occurs, the patient may need either above the knee or below-knee amputation. The purpose of treatment is to save as much of the limb as possible. Blockages of the arteries of the lower limbs may start right from the Abdominal aorta to the vessels of the foot.
The cases outlined below will illustrate the type of blockages which can be treated by Interventional techniques. This treatment is performed in a special laboratory, called the Digital Subtraction Angiography Suite. Most procedures are conducted using a local anesthetic, although in some cases sedation may be used. In the vast majority of cases, the patient may need hospitalization only for a couple of days, for opening up of the arteries. However, if the patient has already developed Gangrene, then treatment of the gangrenous tissue ( if necessary amputation of the affected part) may take a few days more.
Along with Interventional techniques, Hyperbaric Oxygen treatment is also used to increase the blood supply to the affected tissues. In this technique, the patient is placed in a special Hyperbaric Oxygen chamber, and he breathes pure 100% oxygen under pressure for one hour every day. This increases the oxygen content of the blood and delivers increased oxygen to the tissues which are supplied by narrowed or blocked arteries.
_______________________________________________________________________________________
Peripheral Artery Disease
It is a major problem afflicting millions of people in the world. Caused by restricted blood flow to the peripheral arteries, which are situated in the arms, legs, and feet, Peripheral Artery Disease occurs when fatty deposits block blood flow to the feet. The decreased blood flow causes pain and circulation problems that progress and get worse, increasing the risk of stroke, heart attack, and amputation. Peripheral Angioplasty is used to reopen the blocked and narrowed peripheral arteries to restore proper blood circulation. Being a minimally-invasive surgery, the procedure is quite popular for Peripheral Artery Disease.
_______________________________________________________________________________________
Why Do Narrowings Occur?
Most common causes include: Diabetes, cigarette smoking, high blood pressure, and high levels of blood cholesterol. PAOD commonly occurs in the arteries of the lower limbs.
_______________________________________________________________________________________
What Are The Symptoms ?
In the lower limbs, narrowing of the arteries initially leads to pain and cramps in the thighs or calves on walking or climbing stairs. This pain disappears on resting. This type of pain is called ‘intermittent claudication’. Gradually, as the narrowing of the artery gets more severe, the distance in which the person can walk without pain decreases. In severe cases, there will be pain even at rest, usually more at night.
With critical narrowing in the blood vessels, there will be loss of hair over the foot and changes in the nails and skin color. Following an injury, healing may proceed very slowly, leading to the formation of an ulcer. Gangrene soon sets in, with discoloration of the limb, and finally, the limb may need to be amputated. Intermittent claudication is common with advancing age and occurs in about 5% of men and 2.5% of women above the age of 50 years. In about half the patients, the condition will remain stable for many years. One out of four patients, however, will deteriorate, and some will require amputation, especially diabetics and smokers
_______________________________________________________________________________________
How Does One Diagnose This Condition ?
The simplest method of finding out, is the presence of a weak pulse in the affected artery. A special ultrasound test of the arteries (arterial color Doppler test) confirms the diagnosis. The final diagnosis is by performing a special Angiogram called digital subtraction angiography.
_______________________________________________________________________________________
Which Arteries In The Body Can Be Opened ?
Almost any artery of the body which is narrowed or blocked can be opened. The arteries most commonly affected are those of the legs, kidneys, and the brain. Blockages of the arteries of the brain may give rise to episodes of weakness in the face and limbs, and later on to paralysis. In fact, opening up of these vessels (Carotid artery angioplasty) is one of the latest techniques used in preventing paralysis in a significant number of patients.
_______________________________________________________________________________________
When Should Interventional Treatment Be Considered ?
To prevent gangrene and amputation of the limbs, prompt diagnosis and treatment of the arterial narrowing is required. One must strongly consider angiography and angioplasty when :
- Claudication distance gradually decreases – when the patient finds that he can walk smaller distances before stopping due to pain.
- Presence of pain and discomfort at rest.
- Changes in skin colour of the limb.
- Limb starts to become cold as compared to the opposite one.
- Early changes of gangrene. 6) Diabetic foot not responding to usual treatment.
_______________________________________________________________________________________
How Can Surgery Be Avoided ?
It is now possible to treat patients with severe narrowings of the blood vessels with special “interventional techniques”. Under local anesthesia, a small needle is inserted into a leg artery. A thin wire is passed and threaded across the narrowed portion of the artery. A tiny balloon is then positioned and inflated across the narrowing, thereby compressing and flattening the cholesterol blockage. This reopens the artery, and blood flow resumes. This technique is called balloon angioplasty and is similar to what is used in opening the vessels of the heart.
This technique can also be safely performed in elderly, frail people, and patients with severe heart, lung and kidney disease. Balloon angioplasty procedures have a very high success rate. Over a period of time, however, a few of the arteries which have been opened with balloon angioplasty do tend to re-narrow. In general, the larger the blood vessel, the less the chance of re-narrowing occurring. In those cases where the physician suspects a high rate of re-narrowing, “stent implantation” is carried out. Stents are special metallic springs which are introduced within the artery. They act as struts to prop open a blood vessel. Stents are introduced through the same needle hole in the artery and do not require any surgical procedure.
After stent placement, the chance of re narrowing of the artery is very low, and the results rival that of major surgery. Sometimes, the artery is blocked due to a blood clot (thrombus). In such cases, a special plastic tube (catheter) is placed within the artery, at the site of the clot. Through this catheter drugs such as streptokinase, urokinase and Reopro are injected which help to dissolve the blood clot. Following injection of these drugs, additional balloon angioplasty and stenting may be necessary to compress any cholesterol blockages underlying the blood clot in the artery.
_______________________________________________________________________________________
What Are The Benefits As Compared To Surgery?
Interventional treatment of PAOD is done under local anesthesia, and usually, the procedure lasts from half-hour to two hours. Furthermore, most patients can be discharged from the hospital within 24 to 48 hours and can go walking home. There are no cuts, incisions or sutures, so the chances of infection are negligible (especially important in diabetic patients).
Furthermore, most patients who have significant PAOD also have narrowings of the blood vessels of the heart and would be at high risk of surgical operation. In surgery, the blockage is bypassed using a special synthetic graft. Most surgeries are major operations under full general anesthesia, and patients are required to stay in the hospital for at least 7 to 10 days. In addition, the mortality and morbidity rate of surgical procedures is many times that of interventional techniques.
Needless to say, all over the world, interventional techniques for the treatment of PAOD are the procedure of choice. However, there are some cases in which these techniques may not work. In such cases surgical intervention would be required.
Key Procedures
Jaslok Hospital boasts over 300 eminent physicians, many of whom are trailblazers in their specialized domains. Moreover, they have garnered a reputation for devising groundbreaking and inventive clinical protocols.
Find a Doctor/Specialist


